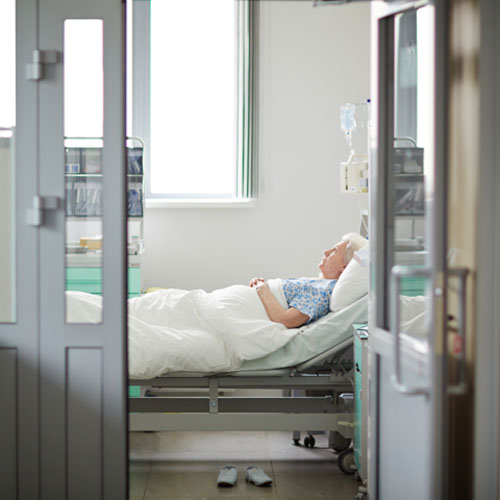
Anna’s hospital allowed only one vaccinated visitor for non-Covid patients per day and only from 10 am to 5 pm. While both parents had flown in to support their adult daughter, as a family, they decided that her mom would be the designated daily visitor and point person with the nurses and doctors. In my role as their patient advocate, Anna’s father and I would stay in the loop virtually during visiting hours via cellphone – the de facto mode of most healthcare communications as public health measures mandate mostly remote caregiving.
The family, already anxious about the grueling surgery to come, was rightfully scared that this new pandemic hospital landscape of curtailed family visiting and overburdened hospital staff could lead to less safe, less attentive care for Anna. To add to their concern, Anna would be flat on her back for the first several days post-surgery.
Anna’s parents wanted to be with her 24/7 following her surgery because she would need them. Who else would devote their full attention to Anna’s well-being? Who knew Anna as a person, not just as a patient, and would be alert to potential signs of deterioration – or improvement? Who would notice Anna’s pain spiking and get her nurse? Who would feed her slowly and patiently throughout the day as she was restricted to a liquid diet; bring her blankets when she was freezing; read to her; hold her hand?
Most critically, who would forge a partnership with her hospital team to assess daily medical updates and be her advocate in formulating the plan of care? Who would talk to her nurses on their hourly check-ins for vitals or when they dispensed medications? Who would confer with Anna’s doctors, especially if they rounded when she was asleep or in no condition to process medical information?
Families aren’t visitors – they are the cornerstone of patient-centered care. During any hospitalization, not just now during Covid, family caregivers are the chief guardians of patient safety for their loved ones. And they, and they alone, are always the providers of essential comfort care – the high-touch in high-tech medicine.
They are also very likely the primary caregivers after discharge to home, and restricting visitors imperils safe discharges to home. Family caregivers routinely assume medical tasks and management of medical equipment at discharge: wound care, emptying drains, managing IVs, dispensing meds, maintaining special equipment, the list goes on. They need that critical time in the hospital to learn: to observe and be trained by staff to carry out duties once home that are not routine but complex and medical in nature.
Most crucially, family is the vital link promoting communication between doctors, nurses, patients, and caregivers. They bring essential insight and knowledge of the patient to inform any medical decision-making process that goes on daily in a hospital setting. While the pandemic has ushered in the rapid adoption of telemedicine and virtual communication, it is not a substitute for family at the bedside continually connecting and collaborating, in essence, building trusting relationships, face-to-face with doctors and nurses.
Cellphones and visitor restrictions are not an adequate substitute for in-person family participation, but this is the reality for the foreseeable future. Given that, we were mindful going in that Anna’s family had to approach the limited 7-hour visiting window proactively. Every minute counted. Anna’s mom needed an essential toolkit to help her organize all the information and personnel she would encounter in the hospital every day.
While I detail a more in-depth, step-by-step plan to manage and monitor a hospital stay safely in The Patient’s Checklist, here are the three simple tips that can maximize opportunities to connect, communicate and collaborate with the care team while visiting restrictions are in place.
Tip 1: Bring a notebook
It’s such a simple but crucial piece of advice and always the first tip suggested by every patient advocate I know. Get a notebook dedicated to your loved one’s hospital stay and write down everything (see tips 2 & 3). Families are unprepared for the overwhelming amount of information, treatments, and personnel encounter during a hospital stay.
Writing it down helps one remember amidst the controlled chaos of the hospital environment. Having notes allows you to review and organize later on, which is the key to clarifying any follow-up questions and concerns to address with your doctors or nurses, whether after visiting hours via phone or the next day in person.
Anna’s mom wrote down everything – she told the story of what happened each day in the hospital:
Who were her daughter’s nurses – the backbone of day-to-day hospital care? Did she see the doctors in person, and if so, what did they say? Were there hours Anna felt better – or worse? Was she able to sleep? Was she in pain? What were her medications? Was her incision healing? Were her catheter and IVs being checked often? What medical tasks would Anna’s mom need to do after discharge – and who would teach her?
We needed this information to strategize how best to care for Anna both in-person and remotely. Every day I would call in several times to talk with Anna and her mom on speakerphone to get updates. Having all her medical information organized in the notebook and at our fingertips made us more effective in communicating concerns when we could not do it face-to-face. We made it a point to talk to her night nurse or her doctors by phone once visiting hours were over.
Anna was usually up to participate in all conversations (and we made sure her cellphone was always fully charged). Still, she could rarely remember what was discussed later, so it was vital that her parents, either in person or remotely, were included in all medical discussions (and took notes). And of course, we had Anna’s permission to gather her medical information and speak on her behalf when necessary.
Tip 2: Get names, contacts, schedules for your hospital team
Anna’s mom wrote down the names and contact numbers for everyone on the care team – she made it her policy to ask everyone who entered her daughter’s room to introduce themselves and tell her what their role was. Anna’s mom noted the number of the nurses’ station on the floor and the name of the person who staffed that desk if she needed to reach her daughter’s nurse after hours.
She also wrote down shift schedules – typically, nurses are on 12-hour shifts while personal care aides are on 8-hour rotations. For the doctors, she noted next to their names their role on the team and their cellphones, office numbers, and when they rounded.
During her daughter’s 8-day hospital stay, Anna’s mom never met any of the nighttime nurses or aides in person as their shifts began and ended when visitors weren’t allowed. Nearly every day, the doctors rounded either before or after visiting hours.
Think about that—no face-to-face conversations with key providers of your loved one’s hospital care. Instead, we had to make virtual communication work for us as best we could.
Together, the family and I devised numerous workarounds. If her doctors rounded after visiting hours, we requested them to call us when they were with Anna. Anna’s mom got to know the night nurse by calling in when medications were being dispensed because she knew the times – see tip 3. None of this was equivalent to building relationships in person, but connecting a voice with a name made virtual communications better if it couldn’t be a face.
Tip 3: Know the medication schedule
Anna’s mom made a comprehensive list of all medications, what they were for, who prescribed them, and the schedule and dosage. If she was there, this was a time she could talk to the nurse about any aspect of Anna’s daily care plan. After visiting hours, she would call Anna when her medications were scheduled to be dispensed to make sure they were on time and to do a check-in with the night nurse to get her input on Anna’s progress.
The second night after surgery, Anna called me. She was alone and in extreme pain – she said a ten on the scale. She had another hour to go before her next dose of pain medication, and she didn’t know what to do. I had Anna use the call bell and put me on speakerphone when her nurse came into the room.
Together we were able to change the pain medication plan because it wasn’t working. The nurse called the attending physician right there and then. They increased her pain medication, and the schedule switched to every three instead of four hours.
Families need to prepare for this new and unfamiliar hybrid form of hospital caregiving: limited in-person engagement supplemented with cellphone communication. The era of family at the bedside around the clock caring for a loved one during a hospital stay may be a permanent casualty of Covid.
These three simple tips help families stay in the loop with the hospital care team, whether in-person or virtually, because staying informed is the key to protecting your loved one during hospitalization.
***
Let’s connect on social! I’m on Twitter, Facebook, and LinkedIn, or by email at [email protected]. Purchase your copy of The Patient’s Checklist here!